Peace Arch Hospital, with the oversight of Fraser Health, is moving forward with plans – among them a new $20-million emergency department – to keep pace with the needs of a rapidly growing and evolving community. In a series of articles launched today, Peace Arch News examines how the hospital came to be, how staff are coping with current challenges and how a new vision for health care in the Semiahmoo Peninsula aims to ensure the hospital remains responsive to the community for years to come.
• • •
It's slow day in emergency at Peace Arch Hospital – and that's a good thing.
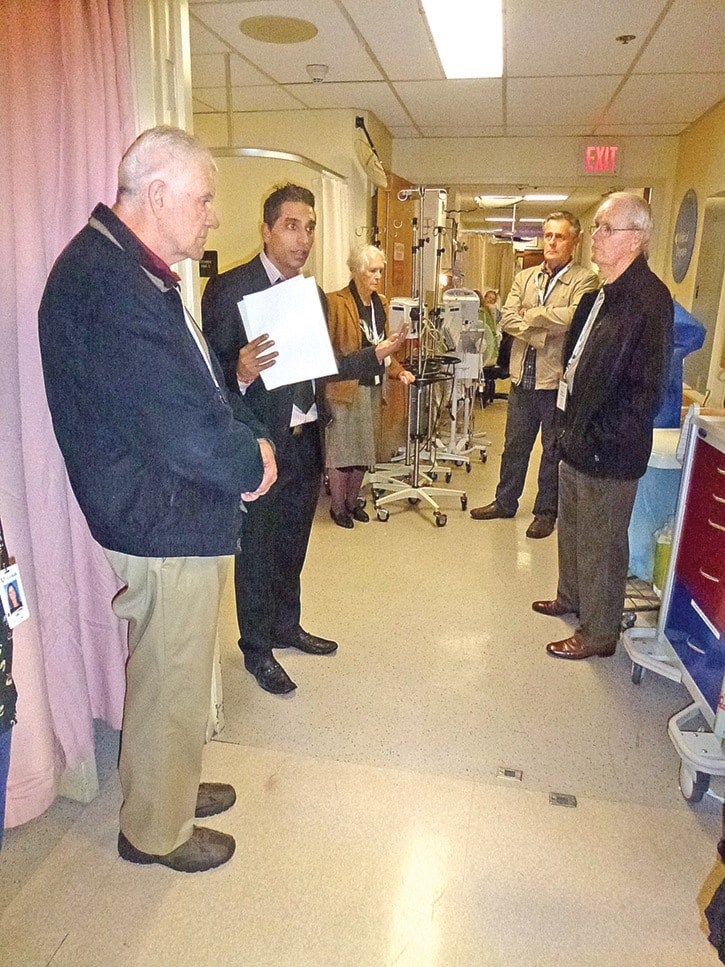
Even so, the dozen of us on a tour of the department with new manager Jessie Saran are conscious of the potential for getting underfoot, although he's guiding us as discreetly as possible, and doctors and nursing staff are calm as they excuse themselves to walk around us.
One gets the feeling they'd be just as professional, and just as polite, if emergency went into 'code orange'. Then they'd be dealing with a crisis situation – an infectious outbreak or some calamity involving multiple injured patients.
Worst-case scenarios come to mind; a train derailment, a freeway pile-up, an aircraft crash or a tsunami.
Even a sudden spate of admissions, including cases demanding immediate attention, would be enough to have us cleared from the area, politely but firmly.
Fortunately, this afternoon the department can handle a visit from community members who, by donating, play an indisputably important part in the system, and the staff's ability to care for patients.
Donations – and other fundraising through the Peace Arch Hospital and Community Health Foundation – have raised more than $9 million – more than two-thirds of the way to the $15 million the community must provide for a new $20-million ER (Fraser Health will contribute $5 million).
That's enough to green-light the project, which is expected to break ground by next summer, with completion set for late 2018-early 2019.
It's a step that's past due. When the existing ER was completed just over a quarter-century ago, it was designed to accommodate 20,000 patients a year. Last year, it treated 50,000. Current projections are that demand will reach the 70,000 annually by 2020.
It's easy to see from today's tour how necessary a new ER is.
Starting with 'triage,' largest area of the current emergency department, where walk-in and ambulance patients are assessed for care when they arrive, donors see a succession of spaces – they can't really be called rooms – where different levels of care are administered.
Most were not specifically designed for their current use; they've been ingeniously repurposed from earlier supply or office use as the number of patients has escalated with a growing community. Some spaces were, quite literally, closets before a bed was moved in.
"Any nook and cranny, it seems like we have patients in there – that's our challenge," our tour guide says.
As Saran explains the function of each area, we can't help glimpsing patients, too. The meeting of eyes is inevitably uncomfortable. After all, whatever problems brought them there are private and confidential – matters that, quite properly, should be between them and their caregivers.
We can't help feeling like intruders when curtains around beds part to reveal frail, vulnerable bodies in thin hospital gowns, or when pale and elderly faces blink at us with curiosity from gurneys and beds set up further down hallways than our tour will reach.
When Saran points to a forest of IV (intravenous injection) poles clustered in a spare corner, it's just another indication how much every available inch of space is utilized.
It's evident our visit – even on a relatively placid day like this – is simply just too many bodies for narrow hallways and rooms built for another era, with a far different set of expectations of what a hospital could or should provide.
The drawbacks of cramped quarters are particularly noticeable in the trauma and resuscitation area, Saran says, where patients need immediate, highly crucial attention.
"You have a lot of team members squished into a small place, working together to save a life," he says. "It becomes very tight, very difficult to get equipment in or out."
As the role of the ER evolves, there are other rooms – not part of the hospital plan when it was first opened in 1954, or even part of the last upgrade in 1989 – that have become increasingly necessary, he says.
"Unfortunately we only have one isolation room. If there were a superbug we'd need to make sure we were containing it. And there's only one seclusion room – mental health issues are on the rise, and we want to make sure we are accommodating this community at the same time, not just putting people into hallways."
As the tour continues, the donor visitors have their questions for Saran: how far ahead the hospital is planning, will new expansion keep pace with projected demand, will cameras provide coverage of every area, will heli-pads be incorporated in future?
Not all can be answered readily. While Saran says use projections have been made up to 2037, planning is a lengthy – and fluid – process, involving not only hospital staff but the oversight, and budgeting approval, of the Fraser Health Authority.
But it's evident this afternoon that what we're seeing, in a way, is not just the situation in emergency but Peace Arch Hospital in microcosm.
"We just don't have the capacity – the community is growing at such a rate," Saran says.
"We want to make sure that we're moving patients area to area so they're in the right space to get the right care. That's our mantra."
Even with current challenges, the team is managing well, he emphasizes.
"This hospital provides teamwork and quality of care like no other," Saran says, noting that while he has only been with Peace Arch since August, he's worked with Fraser Health for 20 years.
"I can't say enough about the people working here."
Even granted Saran's endorsement of the commitment and coping skills of staff, it's evident that it's more than time for the hospital, not simply to expand, but to move forward into a new era.
Next week: ER staff comment on the challenges they face and the planning underway.