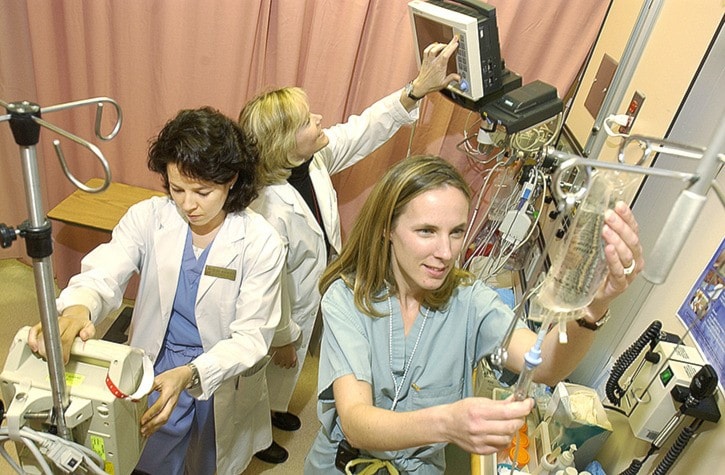
Peace Arch Hospital is moving forward with plans to keep pace with the needs of a rapidly growing community. In the second of a series of articles, Peace Arch News talks to Jennifer McDuff, clinical co-ordinator for the planning of a new $20-million ER, about the day-to-day challenges she sees firsthand as a nurse ,and how a vision of 'patient flow' aims to help the department function for decades to come.
Jennifer McDuff still has vivid memories of the afternoon young Emily Cox was brought to emergency at Peace Arch Hospital.
The eight year-old had been playing at her grandparents' house when she stuck a metal nail file into the socket of a live extension cord.
The immense electric shock sent her into immediate cardiac arrest. For 28 minutes, Emily was clinically dead, while emergency personnel raced against time to airlift her to the hospital and get her into the ER's resuscitation unit.
It was a parent's worst nightmare, but for many ER staff – parents in the same South Surrey-White Rock community – such incidents feel personal, too.
"The doctor and I both had eight-year-old children at that time," McDuff, an ER nurse and clinical nurse educator, said.
"Seeing that little girl on the bed in full cardiac arrest was like looking down and seeing my own daughter… We worked on her for well over an hour. We didn't think we would get her back – but we didn't want to stop."
Witnessing children in such predicaments – which she has done several times in her more than 12 years at PAH – is, McDuff said, among "the biggest, scariest things" she can think of in an area of the hospital where, she acknowledged, "we see some bad things."
The tight-knit, family feeling of Peace Arch Hospital staff is important at such times, she said.
"We hold it together until it's over – and then we cry."
Fortunately, Emily's case had the best outcome one could hope for – today she's a healthy teen who appears in a Peace Arch Hospital fundraising video, with her mom, Liane, to extol the care she received and emphasize the importance of the hospital in a growing area.
And, as McDuff points out, it's an area with a changing demographic – while there are still many seniors, there is a noticeable increase in children and families passing through the hospital.
It's impossible not to feel personally invested, she said, when it's still a small enough community that you could be treating "your mom, your children, your neighbours."
She and her husband, Shawn, live in the area. Their youngest daughter, Sydney, volunteers at the hospital, while Marina is studying at UBC.
Like everyone else, she's seen the changes wrought by the density of burgeoning subdivisions and townhouse complexes, particularly in South Surrey.
"All of those people are going to get sick one day, and they're all going to come here," McDuff she said, with a wry smile.
That's why McDuff, who received her B.Sc. in nursing at UVic and her master's at UBC (she trained as a registered nurse at Vancouver General Hospital ) is happy with her current assignment as clinical co-ordinator of planning the configuration of the hospital's new emergency department.
It's a good fit for her – as someone who educates and mentors other staff on procedures, she's used to communicating needs in pragmatic terms – and she's having fun "playing with the building blocks" of the new ER in an extended consultation with the project architects.
"They needed somebody clinical to say things like 'it doesn't make any sense to have a bathroom there,'" she said.
An area three times the existing ER – including 50 treatment rooms – is just part of the palpable excitement that staff members like McDuff feel about the expansion.
For her it's just as important that a resuscitation area – like the one so critical in saving Emily's life – is planned so that the eight to 12 staff members who may be needed to work with a patient have free access all around the bed; that there are multiple suction and oxygen units; and that all the necessary equipment is mounted on stands or movable booms, rather than being rooted to a single spot.
"That the team can go all around the area – that's going to be huge," she said.
Point-of-care carts at the head of each bed may seem like a smaller detail in equipping a new ER, but it will pay crucial dividends, McDuff said.
"Everything has its place… It saves lots of time spent going back and forth."
A decontamination suite, a five- to six-bed mental health unit with dedicated psychiatric staff and ECG and lab room areas at the front of the new ER – procedures have evolved so that nursing staff are increasingly starting blood work and X-rays for new patients so that it's already there by the time doctors come to see them – are other bonuses of the new plan.
But most important of all is the overall vision: to keep patients continually moving through the hospital to receive the care they need, rather than staying in one room, or – as happens too frequently with the current, crowded ER – receiving care in a hallway.
"We're building it so there can't be stretchers in hallways," McDuff said.
"Even though the department is going to be three times as big, we'll continue with that vision of 'patient flow' so that they're not stuck in emergency. Everything will keep going forward."
It's important to plan with foresight, not just for situations that exist now, McDuff said.
"We have to build for an area that is going to continue to grow – otherwise we'll be back here in 10 years time.
"That's why I wanted this job – to help make the change."
Next week: emergency physician Dr. Jerrod Hendry reflects on his personal stake in the hospital and the community it serves.