Dr. Claudine Storness-Bliss estimates chronic pelvic pain affects about 20 per cent of women worldwide, and of those, about 50 per cent will develop endometriosis.
March is Endometriosis Awareness Month, and there’s still a lot of “under-reporting” when it comes to endometriosis, said Storness-Bliss, an obstetrician-gynecologist and pelvic pain specialist at the Surrey Chronic Pain Clinic at Jim Pattison Outpatient Care and Surgery Centre.
“So many women will talk to their physicians and are told, ‘It’s OK, it’s just your period.’ That’s not quite true when it’s a chronic pain situation that keeps you at home,” she explained.
“Chronic pain is an issue that affects a high percentage of the population, and is unfortunately not well-managed,” said Storness-Bliss.
“It can involve many different organ systems and it’s often difficult to pinpoint what the causes it. You can imagine that proper diagnosis of any actual pathological issue is important and that’s where technology comes in.”
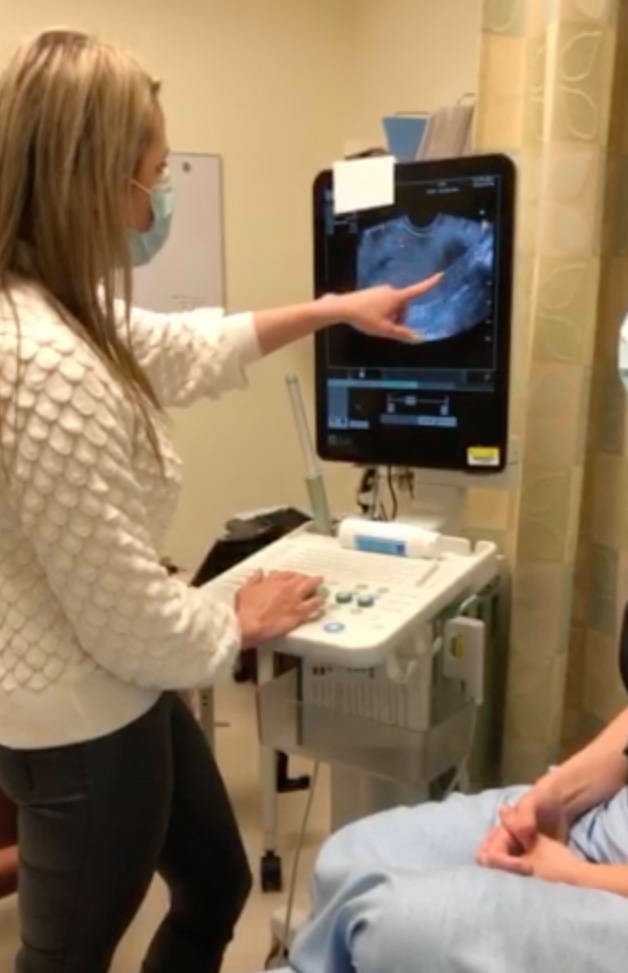
The Surrey Hospitals Foundation has invested $128,000 to help purchase a new 3D-ultrasound machine for the clinic, which is now the only one in the Fraser Health region “with a specialty in treating pelvic pain and endometriosis,” according to a release from SHF.
“Prior to having a 3D ultrasound, I had a 2D machine, which can help diagnose big masses and big problems, but the pelvic adhesions and the smaller pathologies are missed on 2D ultrasounds are now being able to be seen.”
Storness-Bliss said the technology has been around for about a decade, but it “constantly improving every year.” She added the resolution is clearer and she’s able to see the finer details.
“Now it’s become very precise.”
Jennifer Marchbank, a 56-year-old patient of Storness-Bliss, had been dealing with endometriosis for most of her adult life.
“For some women, it causes absolute extreme pain … For me, it was a combination of irregular bleeding, heavy bleeding and a lot of pain,” said Marchbank, a Surrey resident.
With the help of the 3D ultrasound, she said Storness-Bliss was able to properly diagnose her and she underwent minimally invasive surgery.
“She was able to get a good 3D-image, just scanning over my uterus and my belly,” she noted. “In the past, one of the treatments for endometriosis was a hysterectomy and that’s severe surgery.”
It also helps that Surrey now has a chronic pain clinic.
“Can you imagine? I would not have been comfortable travelling in a pandemic to go all the way downtown, nor would it be comfortable to come out for day surgery.”
The only other pelvic pain clinic in the province is at BC Women’s Hospital in Vancouver, Storness-Bliss said. It’s part of the Provincial Health Services Authority, which services all of B.C.
“But, as you can imagine, that’s quite a large number of women to take care of. The Lower Mainland has a really big population, so it was time that we had our own centre and our own technologies.”
lauren.collins@surreynowleader.com
Like us on Facebook Follow us on Instagram and follow Lauren on Twitter